spinal decompression covered by insurance
Introduction
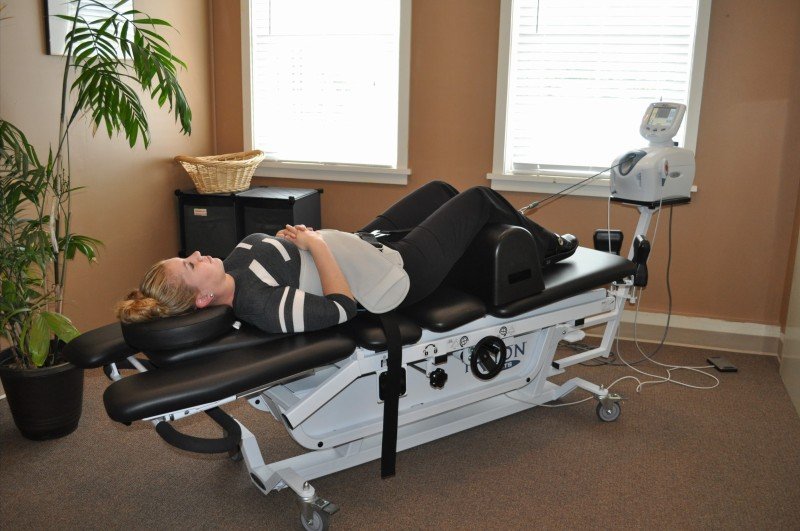
Spinal decompression is a non-invasive therapy that can be used to treat a range of spinal conditions, including herniated discs, degenerative disc disease, and sciatica. While spinal decompression can be an effective treatment option, many people wonder if it is covered by insurance. In this blog, we’ll explore whether spinal decompression is typically covered by insurance and what factors may impact your coverage.
What is spinal decompression?
Spinal decompression is a therapy that uses traction or stretching to relieve pressure on the spine. The therapy works by gently pulling the spine to create space between the vertebrae. This can help to relieve pressure on the spinal discs and nerves, reducing pain and promoting healing.
Is spinal decompression covered by insurance?
Whether or not spinal decompression is covered by insurance will depend on several factors, including your insurance plan, the reason for the treatment, and the type of provider you are seeing. Here are some things to keep in mind:
Insurance plan
The first thing to consider is your insurance plan. Some plans may cover spinal decompression, while others may not. It’s important to review your plan’s coverage details or contact your insurance provider directly to determine if spinal decompression is covered.
Reason for treatment
The reason for your spinal decompression treatment can also impact your coverage. In general, spinal decompression is more likely to be covered if it is being used to treat a medically necessary condition, such as a herniated disc or degenerative disc disease. However, if the treatment is being used for general back pain or other non-specific reasons, it may not be covered.
Type of provider
Finally, the type of provider you are seeing can also impact your coverage. Spinal decompression may be more likely to be covered if it is being provided by a licensed healthcare professional, such as a chiropractor or physical therapist, rather than a non-licensed provider.
What if my insurance doesn’t cover spinal decompression?
If your insurance plan doesn’t cover spinal decompression, there are still options available to you. Many providers offer self-pay options or financing plans to make the treatment more affordable. Additionally, some insurance plans may cover a portion of the treatment or may offer coverage for alternative therapies that could be used in conjunction with spinal decompression, such as acupuncture or massage therapy.
Are there any specific insurance plans that cover spinal decompression?
Some insurance plans may specifically cover spinal decompression as a treatment option. For example, some Medicare Advantage plans may cover spinal decompression therapy for certain conditions, such as herniated discs or spinal stenosis. Additionally, some private insurance plans may offer coverage for spinal decompression as part of their benefits package.
It’s important to review your insurance plan’s coverage details to determine if spinal decompression is covered, and if so, what specific conditions and providers are included. You may also want to speak with your healthcare provider to see if they have any experience working with your insurance plan and whether they can recommend specific providers who accept your insurance.
What are the benefits of spinal decompression?
Spinal decompression can offer several benefits for individuals experiencing back pain or other spinal conditions. Some of the potential benefits of spinal decompression include:
Pain relief: Spinal decompression can help to relieve pressure on the spinal discs and nerves, which can reduce pain and discomfort.
Improved mobility
By reducing pressure on the spine, spinal decompression can help to improve mobility and flexibility, making it easier to perform daily activities.
Non-invasive
Unlike surgical treatments for spinal conditions, spinal decompression is a non-invasive therapy that does not require incisions or anesthesia.
Low risk
Spinal decompression is generally considered a safe treatment option with minimal risk of complications.
Cost-effective
Spinal decompression is typically less expensive than surgical treatments and may be covered by insurance or offered at an affordable self-pay rate.
In conclusion,
whether or not spinal decompression is covered by insurance will depend on your individual insurance plan, the reason for the treatment, and the type of provider you are seeing. If your insurance plan does not cover spinal decompression, there may still be options available to make the treatment more affordable. Be sure to discuss your options with your healthcare provider and insurance provider to determine the best course of action for your individual needs.




